Joint comfort and mobility often feel like a quiet, steady hum under the noise of daily life — and when that hum turns into a complaint, it quickly takes center stage. Good nutrition quietly supports the tissues, fluids, and systems that keep your joints moving smoothly, and a few deliberate food choices can make a measurable difference. If you search for Питание для здоровых суставов, you’ll find advice ranging from fads to well-researched guidance; this article focuses on the latter, combining science, practical tips, and real-life experience.
How joints work and why food matters
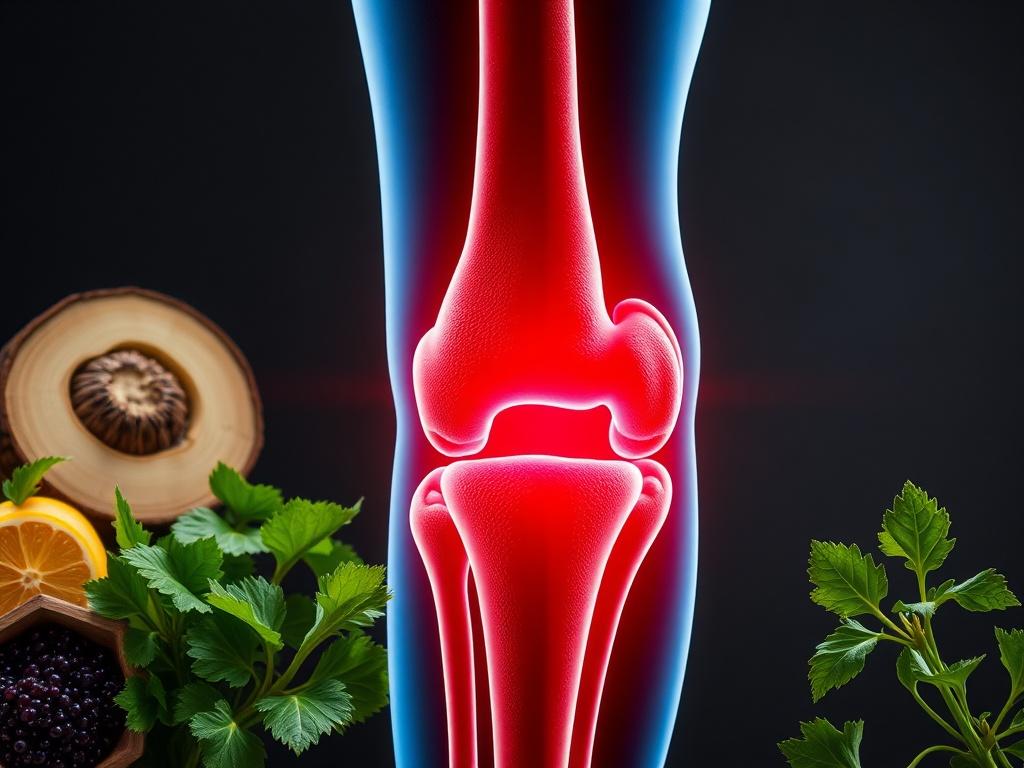
Joints are complex interfaces where bones meet, cushioned by cartilage, lubricated by synovial fluid, and stabilized by ligaments, tendons, and muscles. Nutrition affects each of these components: collagen and proteins build and repair connective tissue; fats and antioxidants influence inflammatory signaling; minerals like calcium and magnesium maintain bone and muscle function. Food also determines body composition and metabolic health, which in turn change load and stress on joints.
Understanding this physiology helps you choose nutrients that support structural repair, modulate inflammation, and maintain a healthy weight. Diet won’t erase severe mechanical damage or autoimmune processes on its own, but it can reduce symptom severity and improve response to other treatments. Think of eating as routine maintenance — small, consistent inputs that keep a complex machine running better over time.
Essential nutrients for joint health
Certain nutrients repeatedly show up in research and clinical recommendations for joint support. These include long-chain omega-3 fatty acids, vitamin D, vitamin C, collagen (or its building blocks), antioxidants, and minerals like calcium and magnesium. Each plays a specific role: some reduce inflammation, others provide raw materials for tissue repair, and still others support bone density and neuromuscular control.
Below I break down the most important nutrients, why they matter, and food sources so you can design meals with intention rather than guesswork. I’ll also touch on supplements where whole-food sources are limited or clinical needs call for higher doses.
Omega-3 fatty acids: calming inflammation
EPA and DHA, the long-chain omega-3s found primarily in fatty fish, reduce the production of inflammatory mediators that can degrade cartilage and amplify pain. Clinical trials commonly show improvement in joint pain and stiffness when people add sufficient omega-3s, especially in inflammatory conditions like rheumatoid arthritis. Plant-based ALA (from flax or chia) can convert to EPA and DHA only inefficiently, so fatty fish or algae-based supplements are usually recommended for therapeutic effect.
A practical target is two servings of fatty fish per week — think salmon, mackerel, sardines, or trout — or a daily fish oil supplement if dietary intake is low. Keep in mind that high-quality supplements, verified by third-party testing for contaminants, reduce risk and ensure adequate dosing.
Collagen, protein, and amino acids
Cartilage and tendons are rich in collagen, a structural protein built from amino acids like glycine, proline, and hydroxyproline. Dietary collagen or hydrolyzed collagen peptides provide these building blocks and may support repair and reduce joint pain when taken consistently. Adequate overall protein intake is also essential; without sufficient protein, the body cannot synthesize collagen or repair injured tissue effectively.
Bone broths, collagen powders, and protein-rich foods such as poultry, eggs, legumes, and dairy are useful strategies. For older adults, aiming for 1.0–1.2 grams of protein per kilogram of body weight per day supports musculoskeletal health and helps preserve muscle mass around painful joints.
Vitamin D and calcium: supporting the skeletal foundation
Vitamin D helps regulate calcium metabolism and supports bone density — a weak skeleton changes joint mechanics and increases pain. Low vitamin D is linked with musculoskeletal pain and worse outcomes in arthritis, and many adults are deficient, especially in northern latitudes or with limited sun exposure. Calcium partners with vitamin D to maintain bone strength, but calcium without vitamin D is less effective.
Fatty fish, fortified dairy or plant milks, and sensible sun exposure provide vitamin D; supplements are often necessary after testing. Dairy, leafy greens, and fortified foods supply calcium, but absorption improves when vitamin D status is adequate and when oxalate-containing foods aren’t the only calcium sources consumed.
Vitamin C and antioxidants: protecting cartilage
Vitamin C is essential for the enzymatic processes that produce collagen, making it a small but vital player in maintaining cartilage integrity. Antioxidants, including vitamin E, polyphenols, and carotenoids, neutralize oxidative stress that can accelerate cartilage breakdown and amplify inflammation. Diets rich in colorful fruits and vegetables consistently correlate with lower markers of systemic inflammation.
Citrus fruits, strawberries, bell peppers, and broccoli are excellent vitamin C sources, while berries, dark leafy greens, and colorful herbs supply a broad antioxidant profile. A practical approach is to fill half your plate with vegetables and a portion of fruit every day to guarantee a steady influx of protective compounds.
Magnesium, zinc, and other minerals
Magnesium aids muscle relaxation, nerve function, and bone health, indirectly influencing joint comfort by improving neuromuscular control. Zinc participates in tissue repair and immune function, while selenium acts as an antioxidant cofactor. Imbalances in these minerals can subtly impair recovery and raise susceptibility to chronic inflammation.
Nuts, seeds, whole grains, legumes, and green vegetables are rich in magnesium and zinc. If you follow a restrictive diet or have digestive conditions that interfere with absorption, targeted testing and supplementation may be warranted under a clinician’s guidance.
Phytonutrients and spices with evidence
Turmeric (curcumin), ginger, and certain flavonoids have well-documented anti-inflammatory effects and may reduce joint pain for some people. Curcumin, the active compound in turmeric, inhibits inflammatory pathways and can be as effective as low-dose NSAIDs in certain studies when formulated for good absorption. Ginger has similar modulatory effects and may ease morning stiffness and pain.
Incorporate spices like turmeric and ginger into cooking, and consider standardized supplements if you need concentrated doses. Combining curcumin with black pepper (piperine) or using formulations designed for bioavailability enhances absorption and clinical effect.
Foods that support healthy joints
Prioritize whole, minimally processed foods that deliver a mix of protein, healthy fats, fiber, vitamins, and minerals. This dietary pattern supports systemic health, reduces chronic low-grade inflammation, and supplies substrates for tissue repair. Below are foods with specific benefits and practical ways to include them.
Rather than a rigid list of “allowed” and “forbidden” foods, think in terms of patterns: more fish, plants, and unprocessed proteins; less refined sugar and industrial seed oils; and an emphasis on variety to cover the full spectrum of micronutrients.
Fatty fish and seafood
Salmon, sardines, mackerel, and trout provide EPA and DHA, vitamin D, and high-quality protein. Including these two to three times a week delivers anti-inflammatory lipids and supports bone and muscle health. Canned fish—preferably in water or olive oil—is an affordable, convenient option that maintains nutrient density.
For vegetarians and vegans, algae-derived omega-3 supplements offer a direct source of DHA and EPA without fish. Pair plant-based omegas with a varied diet to ensure adequate intake of other joint-supporting nutrients.
Colorful fruits and vegetables
Berries, cherries, citrus fruits, cruciferous vegetables, and dark leafy greens bring antioxidants, vitamin C, and polyphenols that blunt oxidative damage. Tart cherries and berries contain anthocyanins linked to reduced joint pain and better recovery after exercise. Regularly rotating the colors on your plate fills nutritional gaps and sustains anti-inflammatory benefits.
Make smoothies with berries and spinach, roast a rainbow of vegetables, or snack on bell pepper strips for a simple boost in joint-protective nutrients. Fresh is great, but frozen preserves nutrients and is often more practical for busy lives.
Nuts, seeds, and healthy oils
Walnuts, flaxseed, and chia seed contribute omega-3s and magnesium, while olive oil and avocados offer monounsaturated fats and polyphenols. Mediterranean-style fats associate with lower systemic inflammation and better joint outcomes in multiple studies. Avoid excessive intake of industrial seed oils high in omega-6 fatty acids when possible.
Use olive oil for dressings and low-heat cooking, sprinkle seeds on yogurt or salads, and keep a small portion of nuts as a daily snack to improve satiety and nutrient intake. These choices also help control refined carbohydrate cravings, which is indirectly beneficial for joints.
Lean protein and legumes
Protein provides amino acids for repair and maintains muscle mass that supports joint alignment. Lean poultry, eggs, legumes, and tofu are excellent choices, and legumes add fiber and plant-based micronutrients that modulate the gut microbiome. A balanced mix of animal and plant proteins helps maintain muscle while diversifying nutrient intake.
Consider legumes three to four times weekly, integrate eggs for versatile quick meals, and choose lean meat portions rather than overemphasizing red or processed meats, which correlate with higher inflammation when consumed in excess.
Bone broth and collagen-rich foods
Bone broth contains collagen, gelatin, and minerals that may benefit joint health, although the evidence is more supportive for collagen peptides taken as supplements. Nevertheless, bone broth is hydrating, warming, and adds amino acids that support connective tissue. Collagen peptides are flavorless and integrate well into smoothies, coffee, or oatmeal.
I’ve used collagen powder in morning coffee during months of heavy training, and it pairs perfectly with a protein-rich breakfast to keep joints feeling better during increased activity. Consistency matters: benefits emerge over weeks, not days.
Foods and habits to limit or avoid
Some dietary patterns promote inflammation or accelerate joint wear. Reducing intake of refined sugars, ultra-processed foods, trans fats, and excessive omega-6-rich oils can decrease systemic inflammation and lower joint pain. It’s not about absolute prohibition, but about making these foods the exception rather than the rule.
Alcohol in excess can interfere with recovery and sleep, while high-sodium diets may increase swelling in sensitive individuals. Processed meats and foods high in added sugars frequently correlate with worse pain and function in observational studies, so limit them for long-term joint health.
Refined carbohydrates and added sugars
Soda, sweets, and refined grain products spike blood sugar and insulin, promoting inflammatory signaling and weight gain. Weight gain increases mechanical stress on weight-bearing joints and can perpetuate pain. Additionally, chronic high-sugar diets may alter the gut microbiome in ways that favor inflammation.
Swap sugary drinks for water or unsweetened teas, replace refined grains with whole grains, and use fruit for dessert to reduce sugar-driven inflammation without sacrificing enjoyment. Small, sustainable swaps compound into meaningful differences over months.
Processed and trans fats
Foods containing partially hydrogenated oils and many commercially fried items contain trans fats linked to systemic inflammation and cardiovascular risk. Even industrial seed oils, when consumed in large excess, can skew the omega-6 to omega-3 ratio and promote pro-inflammatory pathways. Balance is the key — prioritize monounsaturated and omega-3-rich oils instead.
Read labels, avoid items with “partially hydrogenated” in the ingredient list, and limit fried fast foods. Cook at home when possible with olive oil or avocado oil to keep fats healthful and predictable.
How to build joint-friendly meals
Constructing meals that support joints doesn’t require exotic ingredients; focus on balance and variety. Aim to include a source of high-quality protein, healthy fats, and colorful vegetables with each meal, plus a controlled portion of whole grains or starchy vegetables if needed for energy. This pattern provides the nutrients for repair and the anti-inflammatory compounds for daily mitigation.
Portion control is important for weight management, but so is meal timing and protein distribution — spreading protein across meals helps with muscle maintenance and repair. Below are practical meal-building templates and sample recipes you can adapt.
Meal templates
Breakfast: protein (eggs or yogurt), whole-grain carbohydrate or fruit, healthy fat (nuts or avocado), and a vegetable if possible. Lunch: lean protein or legumes, large salad or roasted vegetables, olive oil dressing, and a small whole grain. Dinner: fatty fish or poultry, steamed cruciferous vegetables, and a fiber-rich side like quinoa or sweet potato.
Snacks: nuts with fruit, hummus with raw vegetables, or a small serving of Greek yogurt with berries. These choices keep blood sugar stable and supply nutrients that continuously support recovery and anti-inflammatory balance.
Sample 3-day meal plan for joint support
This three-day plan emphasizes variety, anti-inflammatory ingredients, and realistic preparation times for busy people. Portions will vary by caloric needs, activity level, and medical conditions, so adjust accordingly. I include simple swap options to accommodate vegetarian choices or allergies.
Consider keeping a few go-to staples — a batch of roasted vegetables, cooked beans, and a jar of homemade dressing — to speed up assembly and reduce reliance on convenience foods that may be inflammatory.
| Day | Breakfast | Lunch | Dinner | Snack |
|---|---|---|---|---|
| Day 1 | Greek yogurt with mixed berries, chia seeds, and a drizzle of honey | Salmon salad with mixed greens, avocado, cherry tomatoes, and olive oil vinaigrette | Stir-fry tofu with broccoli, bell pepper, brown rice, and ginger-turmeric sauce | Handful of walnuts and an apple |
| Day 2 | Omelet with spinach, mushrooms, and feta; whole-grain toast | Quinoa bowl with chickpeas, roasted sweet potato, kale, and tahini | Grilled mackerel, roasted Brussels sprouts, and mashed cauliflower | Carrot sticks with hummus |
| Day 3 | Smoothie with collagen peptide, banana, frozen cherries, spinach, and almond milk | Turkey and avocado wrap on whole-grain tortilla with mixed greens | Slow-simmered bone-broth stew with lean beef, root vegetables, and herbs | Greek yogurt with a sprinkle of cinnamon and sliced almonds |
Supplements: evidence, dosing, and safety
Supplements can be useful when diet alone doesn’t meet needs or when clinical evidence supports higher doses for a specific condition. Common supplements for joint health include omega-3 fish oil, collagen peptides, glucosamine, chondroitin, curcumin, vitamin D, and probiotics. Effect sizes vary, and individual response differs, so try one change at a time and monitor effects.
Always discuss supplements with a healthcare professional if you take medications or have chronic conditions; some compounds interact with blood thinners, antiplatelet drugs, or affect blood sugar control. Quality matters — choose brands with third-party testing and transparent ingredient lists.
Omega-3s, collagen, and glucosamine
Omega-3s: 1,000–3,000 mg combined EPA+DHA daily is commonly used in trials for joint pain; dosing depends on symptom severity and recommendation by a clinician. Collagen peptides: 10–15 grams per day is a common supplemental dose showing benefit for joint comfort in some studies. Glucosamine and chondroitin have mixed evidence; some people experience meaningful pain reduction, especially with osteoarthritis, while others do not.
Consistency is key — expect to try a supplement for at least 8–12 weeks before deciding on effectiveness. Keep a simple symptom diary to track changes in pain, stiffness, and function tied to any intervention.
Curcumin and botanical anti-inflammatories
Curcumin supplements formulated for absorption can reduce pain and stiffness in clinical trials. Typical effective doses range from 500 to 1,500 mg per day depending on formulation. Ginger extracts and Boswellia serrata also show promise for reducing inflammatory symptoms in some people.
Start with lower doses to assess tolerance and avoid taking high-dose botanicals alongside certain medications without talking to your clinician. Natural doesn’t always mean safe for everyone, and quality control among herbal supplements varies widely.
Exercise, weight management, and sleep: diet’s partners in crime
No diet acts in isolation. Strength training to build supportive muscle, low-impact cardio for circulation and weight control, and mobility work for joint range of motion amplify the effects of nutrition. Even modest weight loss — 5 to 10 percent of body weight — can produce meaningful reductions in knee and hip pain for people with excess weight.
Sleep and stress management also matter. Poor sleep increases pain sensitivity and inflammation, while high stress alters eating patterns and cytokine profiles. Use diet to support sleep — avoid heavy meals and high sugar before bed — and combine nutrition with consistent movement and restorative sleep for the best joint outcomes.
Types of exercise that help joints
Focus on three pillars: strength training to support alignment, aerobic conditioning for cardiovascular health and weight control, and flexibility or mobility work to preserve range of motion. Low-impact activities like swimming, cycling, and elliptical training work well for painful joints, and progressive resistance training builds muscle without unnecessary joint strain.
Work with a physical therapist for personalized plans if you have significant joint disease. Small, incremental progress avoids flare-ups and builds confidence in movement over time.
Special considerations: autoimmune disease, athletes, and older adults
People with autoimmune joint disease such as rheumatoid arthritis may benefit from anti-inflammatory dietary patterns but often require immunomodulatory medications for disease control. Diet supports symptom management and overall health but is rarely sufficient alone to control systemic autoimmunity. Collaboration with a rheumatologist and a dietitian helps tailor approaches safely.
Athletes need higher calories and protein to support repair and performance; prioritize anti-inflammatory choices while meeting energy demands. Older adults may need more protein and attention to vitamin D and calcium to prevent bone loss and sarcopenia, which indirectly protects joint function by preserving supportive muscle mass.
Grocery shopping, cooking, and meal prep tips
Practical shopping strategies make joint-friendly eating sustainable. Shop the perimeter of the grocery store for produce, fresh proteins, and dairy; choose frozen fruits and vegetables for convenience; read labels to reduce added sugars and trans fats. Planning two to three meals in advance prevents last-minute choices you may later regret.
Cook once, eat twice: roast a tray of vegetables to use across meals, batch-cook grains, and pre-portion protein for easy assembly. Keep a few spice blends on hand — turmeric-ginger mixes, za’atar, or simple garlic-herb rubs — to add variety without extra effort.
- Make a one-week meal list before shopping to reduce impulse purchases.
- Pick shelf-stable omega-3 sources like canned sardines for pantry backup.
- Keep frozen veggies and precooked beans for fast, nutritious meals.
Monitoring progress and when to seek help
Track pain, stiffness, and functional markers like the ability to climb stairs or walk a set distance to objectively evaluate whether dietary changes help. Give any new routine at least six to twelve weeks to show results, with consistent adherence. If pain worsens, mobility declines, or you notice signs of infection, seek medical evaluation promptly.
Nutrition is one part of a comprehensive plan; significant structural damage, nerve impingement, or progressive autoimmune activity needs targeted medical or surgical interventions. Use diet to support the healing path your healthcare team recommends, not as a substitute when advanced care is indicated.
Real-life example: a practical success story

A few years ago I worked with a neighbor, a middle-aged recreational runner who developed persistent knee pain after increasing mileage. She reduced processed carbs, added two fish meals weekly, began daily collagen peptides, and started twice-weekly strength sessions focused on hips and glutes. Within three months her pain dropped enough to resume easy runs, and she regained confidence to progress gradually.
This wasn’t a miraculous cure — it was the compounded effect of weight stabilization, improved muscle support, and a dietary shift toward anti-inflammatory fats and collagen-building nutrients. Her case illustrates how combined lifestyle changes deliver measurable improvements rather than quick fixes.
Practical checklist to get started
Here is a compact checklist to translate knowledge into action. Use it to design your first two weeks, then reassess and iterate based on what’s sustainable and beneficial for you. Small, consistent changes beat dramatic but unsustainable overhauls.
- Add two servings of fatty fish per week or choose a high-quality omega-3 supplement.
- Include a source of lean protein at each meal to support repair and muscle maintenance.
- Fill half your plate with vegetables and include a variety of colors across the week.
- Replace sugary drinks with water or unsweetened herbal tea.
- Try a collagen peptide supplement or bone broth daily for several weeks to evaluate effect.
- Incorporate turmeric and ginger into meals; consider a curcumin supplement if appropriate.
Final thoughts on building habits that last
Improving joint health through diet is not about perfection; it’s about stacking decisions that preserve tissue, reduce inflammation, and support movement. Consistency over months produces more reliable benefits than short-term extremes. Approach changes with curiosity: sample, measure, adjust, and keep the habits that fit your life.
Some issues require medical care beyond nutrition, and that’s perfectly normal. Use food as a powerful, low-risk tool in your joint-care toolkit — paired with movement, sleep, and medical guidance when needed — to maintain mobility and enjoy the activities that matter most to you.